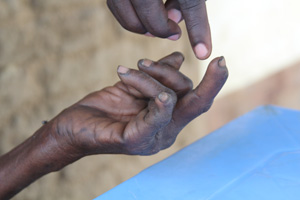
An NCA staff member examines Halima’s hand. If leprosy symptoms are diagnosed early enough, patients do not lose their fingers.
Credits: Sheahen/Caritas
“It started in my right foot. The pain was like a thorn,” says Halima, a widowed grandmother living in a camp in Darfur, Sudan. “Then the illness covered me.”
Most people in the West know of leprosy only from history books and the Bible. The disease is much less contagious than it’s made out to be, and its progress is easily stopped with cheap medicine.
But in a few developing countries, neither the illness nor leper colonies are a thing of the past. For years, hundreds of leprosy patients lived in a place called Towanga near the border of Sudan and Chad. “There wasn’t much food there, but it was enough,” says Mohammad, a healthy 20-year-old man living in the same camp as Halima. “People farmed.” There was also leprosy medication available at a clinic near the border.
Everything changed when violence began in Darfur. Even leprosy patients weren’t spared: Towanga’s residents had to run for their lives. “When we were attacked, I collected clothes and blankets,” says Dahwia, another grandmother in the camp. “We ran on foot, with no shoes. The skin of our feet was raw.”
Dahwia could run because her feet were not damaged by leprosy the way her hands were. The years had taken most of her fingers: “It started with one. Then when that finger was gone, the next finger started,” she remembers. “It happened each season—one more finger would go.”
Dahwia, Halima, and over 500 leprosy patients or their family members made it to Hassa Hissa, a camp for displaced people in central Darfur. “When they came here, the community segregated them,” says Abdul Rahman, a medical staffer at the camp. Exhausted, hungry, and thirsty, the patients and their families were pushed into a corner of the camp.

A woman who is taking tablets after being diagnosed with leprosy examines her hand, which has not been affected.
Credit: Sheahen/Caritas
“In my heart, I felt bad, because we didn’t even get water to drink,” says Dahwia. “The people didn’t let us mix with them.”
During the first chaotic months, “there were no services,” remembers Dahwia. “Doctors here at the camp saw my condition, but didn’t have medicine.”
Muhammad was 14 when he arrived. Because family members of leprosy patients also had to stay in the segregated area, he lived in a tent with seven relatives, including a parent who had leprosy. He and his family couldn’t access leprosy medicine for two years.
People confined to the leprosy area contend with different kinds of prejudice from other camp residents. “I went to Hassa Hissa market, to a place to eat. I washed my hands and entered,” says Muhammad. “Others knew where I was from. They stood up and left their food.”
“It’s not easy for a girl with leprosy to marry,” says Dahwia. Halima’s first husband divorced her when she got leprosy. Both Dahwia and Halima eventually married men who already had leprosy.
Earning money is difficult for everyone in the camp, but especially the leprosy patients. “Even if there’s work available, like washing clothes, people don’t allow us to do it,” says Dahwia. “If a person with leprosy has something to sell, people won’t buy it,” says a 42-year-old man whose name is also Muhammad. “Or if the person wants to clean your house, they won’t allow it.” Some elderly women patients are reduced to begging.
Everyday tasks are, of course, harder for patients who have lost fingers or feeling in their limbs. “If I want to carry a jug of water, cook, stir food, it’s hard,” says Dahwia. “Especially in winter, there was more pain. It’s the same for everyone—when it is very cold or hot, it’s painful,” says Dahwia. “If you’re cooking, it’s very painful to touch fire or cold water.”
With support from ACT/Caritas, local partner Norwegian Church Aid (NCA) began helping this most vulnerable group. To address the basic problem of water, NCA laid pipes and built a tapstand in the area where the patients live.
“If I go to a different water point, I stand far away from it. I’m not allowed to touch the taps,” says Halima. “Someone else fills it. Then I get the plastic jug.
“NCA’s given us services right where we are. There’s no stigma here.”
Because it’s such a challenge for patients to make a living and pay for essential items, the NCA programme also gives aid packages to families affected by leprosy. They receive plastic sheeting, soap, pans, mosquito nets, blankets and more.

Dahwia, a woman who lost most of her fingers to leprosy, receives essential items and medical care from NCA.
Credit: Sheahen/Caritas
NCA provides medical support, such as training family members to properly bind up a leprosy patient’s wounds. Because of stigma, some patients were reluctant to visit certain clinics or even to reveal that they had injuries. The neglected wounds worsened, compounding the problem. NCA gives the community supplies like bandages, gloves, antiseptics, and more. The programme trains volunteers to dress wounds properly at home or in a community centre that NCA repaired.
The NCA programme also teaches people how to recognize the signs of leprosy quickly, because if the disease is caught early on, it can be stopped in its tracks. Since the training, medical assistants have identified new cases and patients have started treatment with tablets provided by the government. One of them, Hawa, holds a package of the tablets in her right hand while examining her left. Both hands are healthy and not deformed, thanks to the medication.
Seeing the patients more cared for has changed perceptions in other parts of the camp. “Now we have an active doctor we can see. We can get medicine,” says Dahwia. “So the other people are nicer to us.”
Stricken with a deforming disease, forced to flee bullets and her longtime home, ostracized even in a camp for displaced people, Dahwia still flashes her perfect smile constantly. “I’ve had many troubles,” she says. “But I’m happy. I’m still alive.”
